Youth's Lives Every Day
Summary
Lesbian, gay, bisexual, transgender, queer, and questioning (LGBTQ) youth are significantly more likely to report depression and suicidality compared to straight/cisgender peers (Johns et al., 2019; Kann et al., 2018). The National Institutes of Health (NIH) has called for research on ways race/ethnicity intersect with LGBTQ identity to impact health disparities (NIH, 2015). However, intersectionality research among LGBTQ youth has been limited due to difficulties obtaining large, diverse samples; and studies that examine race/ethnicity among LGBTQ youth are often limited to comparisons among Hispanic, non-Hispanic White, and Black youth (Mueller et al., 2015), which comprise the majority of the U.S. population. As such, little is known about the mental health of Asian American and Pacific Islander (API) LGBTQ youth. Using data from The Trevor Project’s 2019 National Survey on LGBTQ Youth Mental Health, this brief examines depressed mood, suicidality, and LGBTQ identity disclosure and acceptance among API LGBTQ youth.
Results
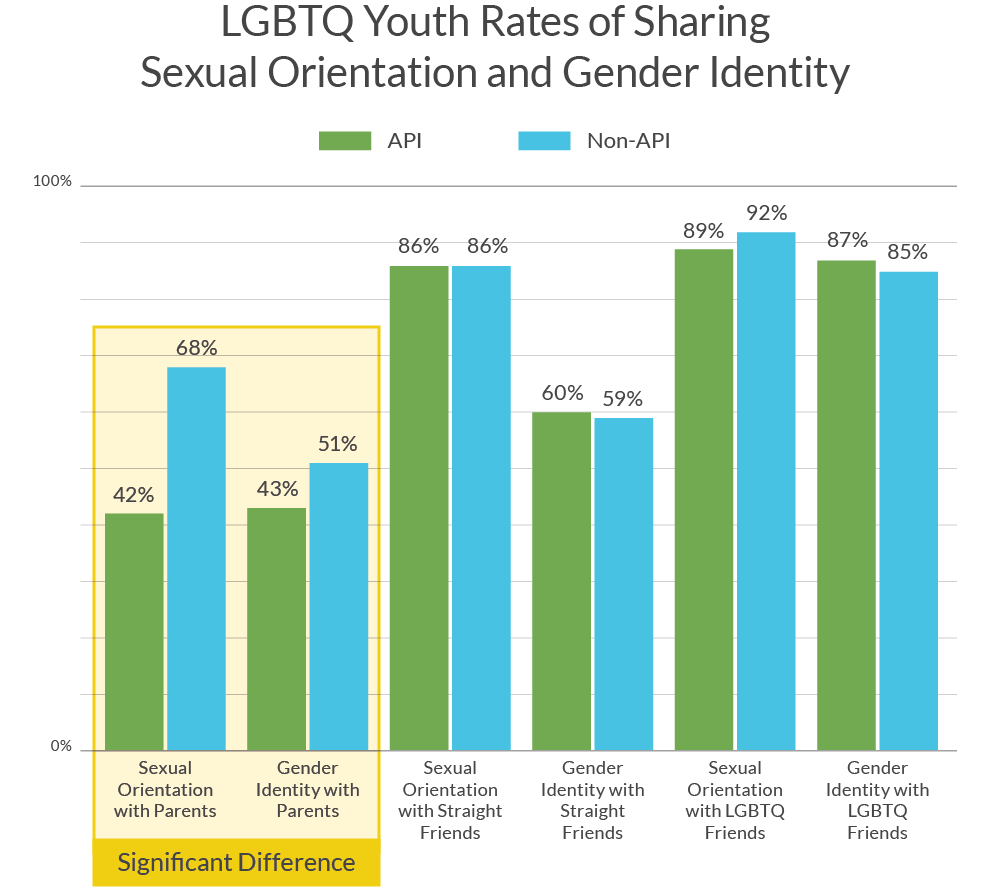
API youth were significantly less likely than non-API youth to share their LGBTQ identity with parents; however, they were just as likely to share with friends. API LGBTQ youth were less likely than non-API LGBTQ youth to share their sexual orientation (42% vs 68%) or gender identity (43% vs. 51%) with parents. API LGBTQ youth reported similar rates to non-API youth of sharing their sexual orientation with straight (86% vs 86%) and LGBTQ friends (89% v. 92%). API TGNB youth also reported similar rates to non-API TGNB youth for sharing their gender identity with straight (60% vs. 59%) and LGBTQ friends (87% vs. 85%).
API LGBTQ youth reported lower rates of depressed mood and suicidality compared to non-API LGBTQ youth. API LGBTQ youth were less likely to report having a depressed mood (60% vs. 71%), seriously considering suicide (33% vs. 39%), or attempting suicide (15% vs. 19%) in the past 12 months compared non-API LGBTQ youth. Transgender and/or nonbinary (TGNB) API youth were three times as likely to report a past year suicide attempt compared to cisgender API LGBQ youth (aOR = 3.02, p<.001).
Most API LGBTQ youth were accepted by friends, and this acceptance reduced the risk of attempting suicide by more than half. Acceptance of sexual orientation from LGBTQ friends (98%) and straight friends (91%) were high and comparable to rates of non-API LGBTQ youth. Rates of gender identity acceptance among API TGNB youth from LGBTQ friends (96%) and straight friends (72%) were also comparable to rates among non-API youth. Sexual orientation acceptance from straight friends reduced the risk for suicide attempts among API LGBTQ youth by more than half (aOR = 0.39, p<.01).
Methodology
A quantitative cross-sectional design was used to collect data through an online survey between February and September 2018. LGBTQ youth ages 13–24 who resided in the U.S. were recruited via targeted ads on social media. A total of 34,808 youth consented to complete The Trevor Project’s 2019 National Survey on LGBTQ Youth Mental Health with a final analytic sample of 25,896, of which 785 identified as exclusively API (youth with family origins in East, Southeast, and Southern Asia and/or Pacific Islands.) Items indicating depressed mood, seriously considering suicide, and attempting suicide in the past 12 months were taken from the CDC’s Youth Risk Behavior Surveillance Survey. Youth were included as “sharing” if they endorsed “your parents,” “your straight friends,” or “your LGBTQ friends,” when asked “Who have you shared your sexual orientation with” or “Who have you shared your gender identity with?” Level of acceptance was rated for each category of individuals with whom they endorsed sharing. Logistic regression models were used to predict attempting suicide, adjusting for age and gender identity.
Looking Ahead
Suicide prevention initiatives should be inclusive of API LGBTQ youth and mindful of the unique findings described in this brief. Although API LGBTQ youth reported slightly lower rates of depressed mood and suicidality compared to non-API LGBTQ youth, their rates were still much higher than those of straight/cisgender youth (Green, Price-Feeney & Dorison, 2020). And API TGNB youth were at three times increased risk for attempting suicide compared to cisgender API LGBQ youth. Acceptance from parents and peers are two of the strongest protective factors for LGBTQ youth mental health (Russell & Fish, 2016). Although API youth were less likely to disclose their LGBTQ identity to parents, most API youth shared their LGBTQ identities and were accepted by friends. Coming out is an incredibly personal decision. There may be certain people with whom youth are comfortable sharing and others with whom they are not. Institutions supporting youth should note Trevor’s Coming Out Handbook, which highlights the importance of youth having the choice to disclose or not disclose their LGBTQ identity. The Trevor Project’s crisis services team supports all LGBTQ youth in their identity, including navigating disclosure, while providing high quality, culturally-grounded care. Further, our research team is committed to using data to assist Trevor and others in better understanding and addressing the needs of API LGBTQ youth.
Recommended Citation: The Trevor Project. (2020). Asian/Pacific Islander LGBTQ Youth Mental Health. https://doi.org/10.70226/DUCO4227
| ReferencesGreen, A.E., Price-Feeney, M. & Dorison, S.H. (2020). Suicidality Disparities by Sexual Identity Persist from Adolescence into Young Adulthood. New York, New York: The Trevor Project. Available at: https://www.thetrevorproject.org/wp-content/uploads/2020/02/Suicidality-Disparities-by-Sexual-Identity-Persist-into-Young-Adulthood.pdfJohns, M.M., Lowry, R., Andrzejewski, J., Barrios, L.C., Zewditu, D., McManus, T., et al. (2019). Transgender identity and experiences of violence victimization, substance use, suicide risk, and sexual risk behaviors among high school student–19 states and large urban school districts, 2017. Morbidity and Mortality Weekly Report, 68(3), 65-71.Kann, L., McManus, T., Harris, W.A., Shanklin, S.L., Flint, K.H.,Queen, B., et al. (2018). Youth risk behavior surveillance-United States, 2017. Morbidity and Mortality Weekly Report Surveillance Summaries, 67(8), 1-114.Mueller, A. S., James, W., Abrutyn, S., & Levin, M. L. (2015). Suicide ideation and bullying among US adolescents: examining the intersections of sexual orientation, gender, and race/ethnicity. American Journal of Public Health, 105(5), 980-985.National Institutes of Health. (2015). NIH FY 2016–2020 strategic plan to advance research on the health and well-being of sexual and gender minorities. Bethesda, MD: National Institutes of Health.Russell, S. T., & Fish, J. N. (2016). Mental health in lesbian, gay, bisexual, and transgender (LGBT) youth. Annual Review of Clinical Psychology, 12, 465-487. |
For more information please contact: [email protected]
© The Trevor Project 2020
