Youth's Lives Every Day
Summary
While many are thriving, lesbian, gay, bisexual, transgender, queer, and questioning (LGBTQ) youth are more likely to report depression and suicidality compared to straight/cisgender peers.1–3 Challenges experienced by LGBTQ youth may be particularly salient for those who are also Black. Mental health concerns are treatable and suicide is preventable. However, being Black in the United States has its own unique experiences coupled with its own specific challenges, and very little is known about how to address the needs of Black LGBTQ youth. Research has documented a variety of challenges faced by Black youth, including post-traumatic stress disorder, depression, and anxiety.4–6 Although mental health concerns have been found in both LGBTQ youth and Black youth, these findings are related to chronic stress stemming from the marginalized social status these individuals have in society.7,8 The intersection of identities for Black LGBTQ youth may make them particularly susceptible to mental health concerns and facing inadequate access to culturally appropriate care. Using data from a large national survey of LGBTQ youth, this brief examines depressed mood, suicidality, and mental health service use among Black LGBTQ youth.
Results
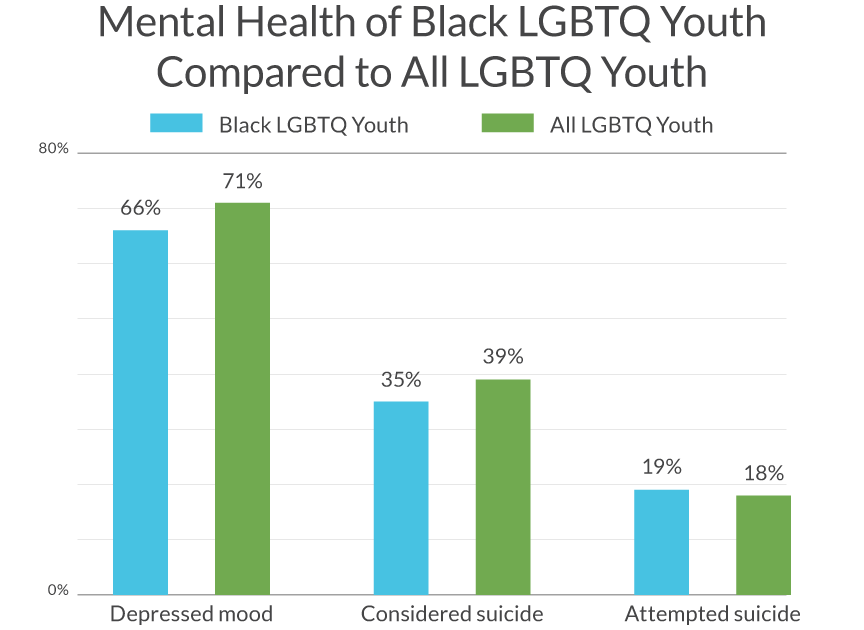
Black LGBTQ youth experience rates of depressed mood and suicidality similar to all LGBTQ youth. Among Black LGBTQ youth in this sample, 66% reported depressed mood in the past 12 months, 35% reported seriously considering suicide in the past 12 months, and 19% reported a past year suicide attempt. These rates are comparable those reported in the overall sample of LGBTQ youth.9 The significantly higher rates of suicidality among transgender and/or non-binary youth in the overall sample are also found among Black transgender and/or non-binary youth. Black transgender and/or non-binary youth reported double the rate of seriously considering (27% vs 59%) and attempting suicide (15% vs 32%) in the past 12 months compared to cisgender Black LGBQ youth. The proportion of transgender and/or non-binary youth seriously considering suicide in the past year was above 50% for each sub-group including transgender women, transgender men, non-binary youth assigned male at birth, and non-binary youth assigned female at birth.
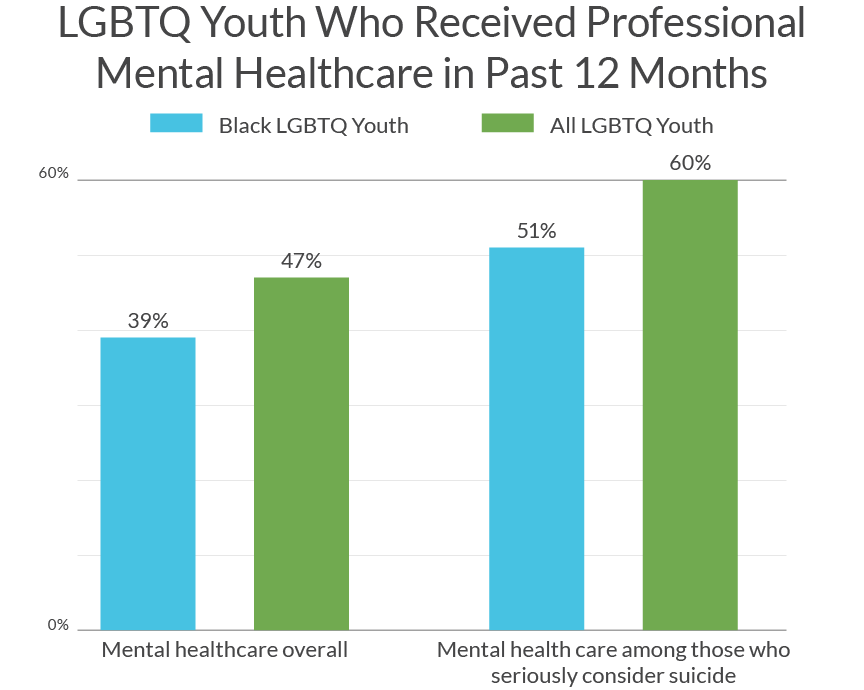
Despite having similar rates of mental health disparities, Black LGBTQ youth are significantly less likely to receive professional care. While 47% of LGBTQ youth overall reported receiving psychological or emotional counseling from a professional in the past year, only 39% of Black LGBTQ youth reported having done so. Among those who seriously considered suicide, only half of Black LGBTQ youth received psychological or emotional counseling compared to 3 out of 5 LGBTQ youth overall.
Methodology
A quantitative cross-sectional design was used to collect data through an online survey platform between February and September 2018. A sample of LGBTQ youth ages 13–24 who resided in the United States were recruited via targeted ads on social media. A total of 34,808 youth consented to complete The Trevor Project’s 2019 National Survey on LGBTQ Youth Mental Health with a final analytic sample of 25,896. The current analyses focused on the 668 youth who reported being “Black or African American,” exclusively. Items indicating past 12 months depressed mood (“sad or hopeless almost every day for two weeks or more in a row that you stopped doing some usual activities,”) seriously considering suicide, and attempting suicide were taken from the CDC’s Youth Risk Behavior Surveillance Survey. Youth were also asked whether they, “received psychological or emotional counseling from a mental health professional?” in the past 12 months.
Looking Ahead
These findings not only support investment in Black LGBTQ youth mental health, but also development and wide application of community-derived prevention programs in which key stakeholders including respected community and church leaders; parents, grandparents, and other family members; and Black LGBTQ youth themselves are included in the process. Black LGBTQ youth are just as likely to experience suicidality as other LGBTQ youth, with over a third seriously considering suicide in the past year and 1 in 5 reporting an attempt. However, Black LGBTQ youth are accessing professional care at lower rates, suggesting existing models of care have failed at providing Black LGBTQ youth access to appropriate and acceptable mental health services. Indeed, most suicide prevention programs for youth often take a “one-size-fits-all approach” and lack the cultural grounding necessary for effective prevention in Black LGBTQ youth.10
The Trevor Project’s crisis services team aims to provide LGBTQ youth with high quality, culturally-grounded care. To better support Black LGBTQ youth we have worked to create a diverse team of counselors that is aligned with the demographics of the youth we serve. We also use counselor training materials that are inclusive of diverse identities, and avoid stereotypes. Our research team is committed to ongoing dissemination of data that allows Trevor and others to better understand and address the needs of Black LGBTQ youth. Further, Trevor’s advocacy team continues to focus on promoting data collection on sexual orientation and gender identity as part of violent death investigations to accurately count and understand violent deaths, including suicide, among Black LGBTQ individuals.
Recommended Citation: The Trevor Project. (2020). Black LGBTQ Youth Mental Health. https://doi.org/10.70226/DWTA1666
| ReferencesBostwick, W. B., Meyer, I., Aranda, F., Russell, S., Hughes, T., Birkett, M., & Mustanski, B. (2014). Mental health and suicidality among racially/ethnically diverse sexual minority youths. American Journal of Public Health, 104(6), 1129-1136.Kann, L., McManus, T., Harris, W.A., Shanklin, S.L., Flint, K.H.,Queen, B., et al. (2018). Youth risk behavior surveillance-United States, 2017. Morbidity and Mortality Weekly Report Surveillance Summaries, 67(8), 1-114.Stettler, N.M., & Katz, L.F. (2017). Minority stress, emotion regulation, and the parenting of sexual minority youth. Journal of GLBT Family Studies, 13(4), 380-400.Alim, T., Graves, E., Mellman, T., Aigbogun, N., Gray, E., Lawson, W., & Charney, D. (2006). Trauma exposure, posttraumatic stress disorder and depression in an African-American primary care population. Journal of the National Medical Association, 98(10), 1630-1636.Walsemann, K. M., Gee, G. C., & Geronimus, A. T. (2009). Ethnic differences in trajectories of depressive symptoms: disadvantage in family background, high school experiences, and adult characteristics. Journal of Health and Social Behavior, 50(1), 82-98.William, D.R., Gonzáles, H.M., Neighbors, H., Nesse, R., Abelson, J.M., Sweetman, J., Jackson, J.S. (2007). Prevalence and distribution of major depressive disorder in African Americans, Caribbean blacks, and non-Hispanic whites: results from the National Survey of American Life. Archives of General Psychiatry. 64(3),305–315.Jones, S. C. T., & Neblett, E. W. (2017). Future directions in research on racism-related stress and racial-ethnic protective factors for Black Youth. Journal of Clinical Child and Adolescent Psychology, 46(5), 754-766.Meyer, I.H. (2003). Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: conceptual issues and research evidence. Psychological Bulletin, 129( 5), 674-697.The Trevor Project. (2019). National Survey on LGBTQ Mental Health. New York, New York: The Trevor Project.Bluehen-Unger, R.G., Stiles, D.A., Falconer, J., Grant, T.R., Boney, E.J., & Brunner, K.K. (2017). An exploration of culturally grounded youth suicide prevention programs for Native American and African American Youth. International Journal of Learning, Teaching and Educational Research, 16(2), 48-61. |
For more information please contact: [email protected]
© The Trevor Project 2020
